Participant Support Procedures > Mealtime Management Procedure
Authorised by Chief Executive Officer
Revised date: 27 July 2023
Review date: 27 July 2024
This procedure explains how Kyeema Support Services will implement mealtime management to participants who require assistance to manage mealtimes (such as those with severe or mild dysphagia, diabetes, food allergies, anaphylaxis or other chronic health risks). It deals with the nutritional value and texture of meals, and with their planning, preparation and delivery.
This procedure supports Kyeema Support Services to apply Standard 4: Provision of Supports Environment – Mealtime Management
Related legislation and policy
NDIS Quality and Safeguarding Practice Standards 2021
NDIS Practice Standards: skills descriptors information for auditors and providers 2018
NDIS (Quality Indicators) Guidelines 2021
Definitions
A Mealtime Management Plan is a plan which prescribes specific support recommendations for the person to eat and drink in a safe and nutritious way.
Procedure
Each participant who needs mealtime management is identified, assessed and has an appropriate mealtime management plan put in place. It also deals with the nutritional value and texture of meals, and concerns the planning, preparation and delivery of meals.
1. Each participant requiring mealtime management is identified
o on their NDIS plan, a concern raised by a carer or via a support worker
o funding is organised with or on behalf of the participant by the Local Area Coordinator, Team Leader or Support Coordinator
o check to see if the participant already has a current mealtime management plan with residential provider or qualified health practitioner
2. With their consent, the participant is referred to a qualified health practitioner for assessment (if no up to date mealtime plan is available)
o refer to Referrals to Allied Health Services Procedure
o comprehensive assessment is undertaken of their nutrition and swallowing requirements; and assessing their seating and positioning requirements for eating and drinking
o check consent forms are current and signed
o participants with severe dysphagia must have a specific health support plan – from a qualified health practitioner. This information may be transferred onto a residential provider form or Kyeema CCF-83 form.
3. The participant is given an appropriate mealtime management plan
o which has been developed in consultation with the participant reflecting their preferences, informed choice and health practitioners recommendations
o which outline their mealtime management needs, including for swallowing, eating and drinking
4. The mealtime management plan can be from a doctor or allied health professional or from residential providers and may be transferred onto a Kyeema Health Support Plan template
o Health Support Plan – Mealtime Management or Dysphagia Support CCF- 83
o Health Support Plan – Diabetes CCF-56
o Health Support Plan – General CCF-44 (anaphylaxis, food allergies, obesity or underweight or other chronic health risk)
5. The mealtime management plan is read and understood by all workers supporting the participant
o workers sign the plan after reading and understanding
o worker signatures are filed in participants file under HEALTH
o workers undergo appropriate training
6. At Kyeema, meals are generally provided by carers, some workers prepare meals in the participants home or cooking programs
o check that the meals provided are of the correct texture, as identified in the plan
o workers prepare and provide texture-modified food and fluids as per the mealtime plan (refer to preparation of texture modified food below)
7. Meals are stored safely
o in accordance with current health standards
o each participant meal is easily identified with labels
o workers are trained in food safety
8. Current mealtime management plans are available to all workers where participant’s meals are prepared and provided. A copy is filed in participants health support files using either
o Kyeema forms CCF Health Support Plan templates
o medical forms from doctor and allied health professionals
o forms from residential providers
9. Day activity lunch areas have a list of participants that are at risk of choking and/or have allergies
o Notes for Lunchroom – Meals, Allergies (K:\DayPrograms\Day Activities 2023\General Day Program Files\Health alerts)
10. Proactively manage the risk to participants with chronic health issues such as:
o swallowing difficulties, diabetes, anaphylaxis, food allergies, obesity or being underweight
o if needs change or difficulty is observed team leaders and/or manager are notified
o workers to immediately seek medical attention when they observe a problem such as when the person appears to have difficulty eating or swallowing their food or drink and/or appears to be in any pain or discomfort
o report incident to the manager/team leader
11. Monitor oral health and ensure good oral hygiene. Report any observations/changes to manager/team leader for follow up with a doctor or dentist
12. Assessments are conducted in a regularly and timely manner
o annually or in accordance with the health practitioner’s recommendations
o workers provide ongoing review via shift notes on Carelink
Preparation of texture modified food
Texture modified meals
Texture modified foods may be thickened, minced or pureed. Due to the extra handling involved with the preparation of texture-modified foods, there is an increased potential for cross contamination.
Cleaning and sanitising equipment
Equipment used to homogenise food usually requires complete disassembly to fully clean.
Procedure for preparing texture modified foods
•Wash hands thoroughly with soap and warm water and dry thoroughly – clean gloves may be used as an additional barrier.
•Texture modified foods should be prepared according to the directions for use of the thickening agent or recipe. In some cases, a blender might be required to achieve an adequate mix.
•Any equipment such as blenders and stab mixers should be dismantled to enable thorough and effective cleaning and sanitising
Where food is modified or puréed without cooking:
For food that is texture modified and not intended to be cooked (e.g. puréed fruit):
•Use equipment dedicated to uncooked ready-to-eat foods only
•Ensure all equipment is clean and sanitised prior to modifying/puréeing
•Ensure these foods are processed before other foods that need to be cooked
•Ensure the equipment is cleaned and sanitised in between uses
Where food is modified or puréed before cooking:
For food that is texture modified prior to being cooked:
•Minimise the amount of time between texture modification and cooking (e.g. less than 1 hour)
•Thoroughly cook food to temperatures of at least 70°C for 2 minutes (or use an equivalent process)
•Ensure texture modified food remains above 60°C before serving.
Where food is modified or puréed after cooking:
For food that is intended to be texture modified after cooking:
•Thoroughly cook food to temperatures of at least 70°C for 2 minutes (or use an equivalent process)
•To limit the risk of contaminating foods that are thickened, puréed or cut up after cooking: – process food in an area away from raw meats and other non ready-to-eat foods on equipment dedicated to ready to-eat foods only
•Texture modify or purée food immediately after cooking
•Ensure food is cooled in compliance with Food Standards Code requirements (the ‘2- hour/4-hour cooling rule’) such that the food is cooled:
– within two hours—from 60°C to 21°C
– within a further four hours— from 21°C to 5°C
– then modified once cooled
•Ensure all equipment has been dismantled, cleaned and sanitised before use
•Minimise the amount of time it takes to texture modify the food before chilling (e.g. place in cool room as soon as possible)
•Minimise the amount of time texture modified food is stored between cooking and reheating:
– Refrigeration should be limited to 48 hours at 5°C or below
– Frozen food should be used within 48 hours of being thawed
•Foods should be reheated to 70°C for 2 minutes (or equivalent) prior to serving.
•Serve reheated food above 60°C
Source: texture_modified_foods.pdf (nsw.gov.au)
International Dysphagia Diet Standardisation Initiative (IDDSI)
From May 1, 2019, Australia has been following the International Dysphagia Diet Standardisation (IDDSI) framework www.iddsi.org. This is a change from the Australian Food Texture Scale previously utilised. The International Dysphagia Diet Standards have introduced levels of texture modification for liquids and modified texture foods.
The new standards have been introduced to ensure consistency of texture by creating a series of simple, yet reliable tests for each level of texture modification. A speech pathologist will review the condition and request food be texture modified only to the level the person can safely manage, and no more.
Instructions on ensuring that meals are of the correct texture as identified in plans - A person’s level of texture modified food may change over time – upgraded or downgraded – so being aware of the person’s current status is crucial - International Dysphagia Diet Standardisation Initiative. https://iddsi.org/'
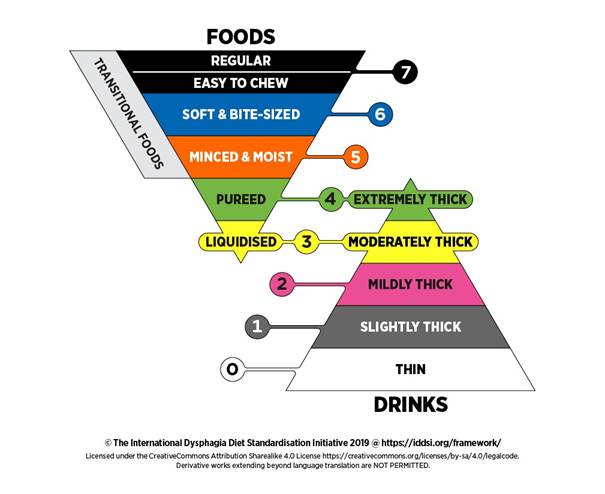
The IDDSI food and drink modification levels go from level 0 to level 7. It is important that workers follow the participants current mealtime management plan and check that the food is the correct level for the participant, as identified in the plan.
IDSSI Food levels:
Level 7 - Regular:
Food is easy to chew.
Level 6 - Soft:
Food may be naturally soft or may be cooked or cut to alter its texture; can be chewed with minimal effort.
Level 5 - Minced and Moist:
Food is soft, moist and easily mashed with a fork; lumps are smooth and rounded.
Level 4 - Smooth Purée:
Food is smooth, moist and lump free; may have a grainy quality.
Level 3 - Liquidised

IDDSI Fork Pressure Test
It is safest to test food using the IDDSI Fork Pressure Test. Here is an example of how to test Level 6 Soft & Bite Sized for Adults.
Level 6

Training
General training is provided to all support workers on food safety and meal preparation:
•Annual Refresher Training - International Dysphagia Diet www.iddsi.org
•First Aid & CPR
•Sentrient: Food Safety – food handling course
Specific training is provided to all workers, including the high intensity workers who support participants with a dysphagia support plan (Sentrient):
•Complex Care - Advanced Mealtime Management (Advanced Mealtime Management covers the basics of supporting people with disability at mealtimes. It looks at nutrition, swallowing, food preparation, and most importantly, safety during mealtimes)
•HISW- Complex Care – Severe Dysphagia Management (Learners will understand the importance of following a person’s mealtime management plan and always working within the scope of practice, and demonstrating a duty of care towards those they support).
•HISW- Dysphagia- Modified Food & Fluids IDDSI poster
High intensity workers have annual refresher training and refresher training if they have been absent for 3 months or more:
•HISW – Complex Care – Mealtime Refresher
•HISW – Complex Care – Severe Dysphagia Refresher
In addition, high intensity workers have:
•Individual Training Plans
•High Intensity Support Worker Skills Review – Severe Dysphagia CCF-54
Review and Evaluation
Occurs annually or in accordance with the health practitioner’s recommendations.
If any changes are observed, then a review may be required earlier.
Responsibilities
Any mistake or error in providing direct health supports is reported immediately to the supervisor and the Incident Reporting Policy and Procedure followed.
Record keeping
Workers
Kyeema maintains a database of trained workers and the direct health supports they are trained to provide:
•Sentrient – Learning Management System (LMS)
•K:\General Items for All Staff\Databases\Staff Training Database
Individual Training Plans
•Electronic records on Sentrient
•Hard copy files (folder kept in HR/Training Office)
•Archived records – K:\Admin\Training\2023 High Intensity Supports ITP High Intensity Support Worker
Skills Review – Severe Dysphagia CCF-54
•Electronic records on Sentrient
•Hard copy files (folder kept in HR/Training Office)
Participants Health Support Plans
Hard copy:
•Participant health support plans are kept in the locked filing cabinets in the team leader area
•Evidence that workers have read the health support plans are kept with the participant files
o CCF-59 Staff Acknowledgement – Health Support Plan
Electronic copy: K-drive\Client or Participants\Adult
•Go to adults name
•Go to health folder
K-drive\ Client or Participants\Children & Adolescents
•Go to young person’s name
•Go to health folder
Complaints
Kyeema service issue complaints refer to Complaints and Feedback Management Policy and Procedure
Related Policies, Procedures and Documents:
Consent to Exchange Information and Use Photos CCF-01
Participant Choice to Engage in Risk Eating CCF-27
Consent to Share Information - Easy Read CCF-57
Staff Acknowledgement – Health Support Plan CCF-59
Health Support Plan – Mealtime Management or Dysphagia Support CCF- 83
Health Support Plan – Diabetes CCF-56
Health Support Plan – General CCF-44
High Intensity Support Worker Skills Review – Severe Dysphagia CCF-54
Medication Checklist – Daily Medication CCF-33
Support Planning Process - NDIS Documentation Flowchart CCF-84
Support Planning Process - TAC Documentation Flowchart CCF-85
Non-Prescription OTC Medication Record Form CCF-98
High Intensity Supports Procedure
Incident Reporting Policy and Procedure
Code of Conduct NDIS/TAC etc - Workers
Privacy and Confidentiality Policy and Procedure
Referrals to Allied Health Services Procedure
Individual Training Plan
Notes for Lunchroom – Meals, Allergies (K:\DayPrograms\Day Activities 2023\General DayProgram Files\Health alerts)